WASHINGTON, 20 January 2006 (RFE/RL) – Volunteers at the University of Maryland near Washington, D.C., participated in trials this month to test the effectiveness of a new experimental bird-flu vaccine. The vaccine was developed from a sample H5N1 strain of the virus taken from a Vietnamese patient in 2004.
So far, the preliminary data from the test looks encouraging. That’s because the experimental vaccine did provoke an immune response in the volunteers -- the kind of response that can enable a body fight off an infection. But scientists do not know whether this experimental vaccine would be even partially effective against new virus strains were H5N1 to mutate.
"The problem is that the strain of the disease that will allow human to human transmission -- which is really the serious problem that we're worried about -- doesn't exist yet," Maureen Lewis, a senior fellow at the Washington-based Center for Global Development, explains. "So we can't really develop a vaccine against that or an effective treatment because we don't know exactly what it looks like. And viruses are notoriously unstable."
According to Lewis, scientists learned valuable lessons from an earlier global health scare, sudden acute respiratory syndrome (SARS). That flu-like illness started in China and eventually swept through 25 other countries from late 2002 to 2003.
"The world community actually did a lot of research on SARS when it emerged," Lewis says. "And, you almost had a competition among the laboratories to figure out what the genome structure was so that they could develop a vaccine. And they did. And they did it very quickly. And in a sense, they are trying to do that now."
But as scientists now face the challenge of developing a vaccine against bird flu -- and particularly against a form of human-to-human transmitted bird flu that has yet to emerge -- they are discovering this particular disease presents its own surprises.
For example, they have found that even trying to protecting people against the current form of H5N1 carried by animals requires large amounts of the experimental vaccine.
"The research that has been done so far has been very helpful in that it has shown us that when you make a vaccine the conventional way against H5N1 you have to use a lot more vaccine to get people to respond to it," says Dr. Andrew T. Pavia, chairman of the national public health committee of the Infectious Diseases Society of America and chief of pediatric infectious diseases at the University of Utah.
"And, that was an important lesson, although a very disappointing and scary one," Pavia adds. "And, so now there is a great deal of research going on to try and make vaccines that are more efficient, so that you don't have to produce a lot more protein to put in somebody's arm in order to get a response. Hopefully, we will have those details worked out before we have to face an efficiently transmitted human-to-human H5N1."
Any disease that requires large doses of vaccine for protection presents a problem because, everywhere in the world, the pharmaceutical sector’s capacity for producing vaccines is limited.
"Currently the world capability is somewhere less than 500 million doses of vaccine with, you know, close to 6 billion people in the world," Dr. Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases in Washington, explains. "In addition, the dose that's required to induce an immune response with this particular vaccine is a significantly higher dose than the dose that you use to protect against the standard run-of-the-mill seasonal flu."
Fauci says that U.S. government officials are concerned not only about inadequate manufacturing capacity but also about where that capacity is located. "We are tending much more towards making sure that we have pharmaceutical plants that are located on U.S. soil, so that we don't have a situation where if you have a global pandemic, then countries would obviously be nationalizing [their] factories," he says. "So, we want to work with other companies. We want to work with other countries. We want to work with international as well as domestic companies, but we don't want to have everything that we are doing be done outside of the United States, which is almost what is the situation right now."
The Canadian government has already -- theoretically -- lined up enough vaccine supply for its citizens. It concluded a 10-year contract with a domestic supplier that is intended to ensure that there is enough bird-flu vaccine -- once an effective vaccine is found -- for every Canadian to receive a dose.
However, countries such as Armenia, Ukraine, and Georgia have no domestic vaccine manufacturers, in part because vaccine production was concentrated in Russia during the Soviet era. But even Russia may have to depend on the largesse of the World Health Organization and other countries. Experts question whether Russian companies have the technical know-how, quality, and regulatory controls in place to produce a new vaccine quickly.
Affected Areas
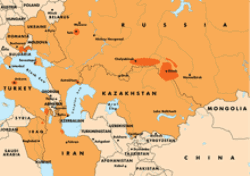
Click on the map for a closer view of the areas within RFE/RL's broadcast region where cases of diseased fowl have been confirmed. Last updated on February 20.
BIRD FLU, or avian influenza, continues to menace scattered areas from East Asia, where the disease first appeared, to Southeastern and Eastern Europe and beyond. Authorities around the world are bracing themselves -- and, more importantly, planning and taking measures to fight the disease wherever it appears.
Stories Of Particular Interest:
Bird-Flu Expert Discusses Issue Of Migratory Birds
Bird Flu: As European Worries Grow, Some See Benefits In Alarm




